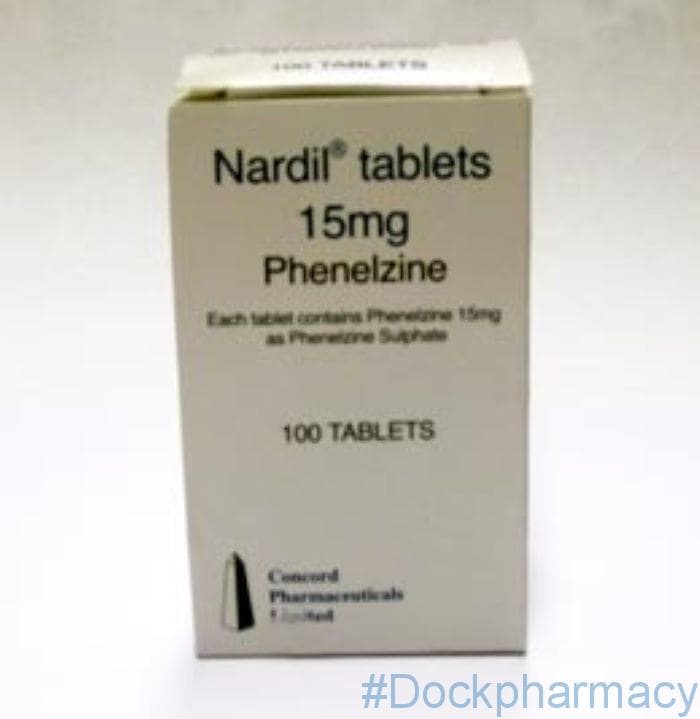
Nardil 15mg Tablets – Phenelzine, 100 Tablets
Nardil 15mg Tablets 100 Tablets
Nardil contains the active ingredient phenelzine, which belongs to a group of medicines called monoamine oxidase inhibitors, or MAOIs.
Nardil is used to treat certain types of depression. It works by changing the way messages are sent from one nerve to another in the brain. Nardil is especially helpful when:
- depression does not follow the typical pattern
- anxiety or fear is a main symptom
- treatment with other antidepressants has failed.
Nardil patient information leaflet
Original price was: £195.50.£178.00Current price is: £178.00.
CompareCompareNardil 15mg Tablets 100 Tablets
Nardil contains the active ingredient phenelzine, which belongs to a group of medicines called monoamine oxidase inhibitors, or MAOIs.Nardil is used to treat certain types of depression. It works by changing the way messages are sent from one nerve to another in the brain. Nardil is especially helpful when:- depression does not follow the typical pattern
- anxiety or fear is a main symptom
- treatment with other antidepressants has failed.
Nardil 15mg Tablets 100 Tablets
Nardil Tablets is used to treat certain types of depression:
- depression does not follow the typical pattern
- anxiety or fear is a main symptom
- treatment with other antidepressants has failed.
Brand
Nardil
How To Use
The usual starting dose is one tablet three times a day. Your doctor will decide what dose is best for you. Follow the instructions on the label and do not change the dose unless your doctor tells you to.
Swallow the tablets with some water. You can take them with or without food.
Your blood pressure should be checked frequently by your doctor and Nardil should be stopped if palpitations or frequent headaches occur.
Ingredient
Nardil tablets contains the active ingredient phenelzine, which belongs to a group of medicines called monoamine oxidase inhibitors, or MAOIs.
Warnings
Do not take Nardil 15mg Tablets and tell your doctor or pharmacist if any of the following applies to you:
- an allergy to phenelzine or any of the other ingredients of Nardil (see Section 6 or end of Section 2 “Important information about some of the ingredients of Nardil Tablets”)
- a growth on the adrenal glands near your kidneys which is causing high blood pressure (phaeochromocytoma)
- liver disease – now or in the past
- a disease affecting blood supply to your brain, such as stroke
- heart disease
- you are in a manic phase
- you are pregnant or breast-feeding
- you are below 16 years of age
- you are already taking, or have recently stopped, other antidepressants ie. MAOIs, tricyclics, Selective Serotonin Re-uptake Inhibitors (SSRI) or Serotonin Noradrenaline Re-uptake Inhibitors (SNRI). It is important to wait between using certain antidepressants and starting Nardil Tablets, read section 2: Taking other medicines carefully.
- you are taking strong pain killers, such as morphine or pethidine
- you are taking guanethidine (used to treat high blood pressure), dextromethorphan (used in cough and cold medicines) or medicines which affect the central nervous system and make you feel sleepy.
If any of these apply to you, tell your doctor or pharmacist before taking Nardil tablets.
Take special care with Nardil tablets
You should consult your doctor or pharmacist before taking Nardil if you have any of the following conditions:
- agitation
- epilepsy
- porphyria (which may make the skin sensitive to sunlight, or may affect the nervous system, causing abdominal pain, vomiting, muscle weakness, fits and mental disturbances)
- abnormalities of blood cells, this could be caused by many different diseases and symptoms can include bleeding problems, weakness or pale skin colour, or frequent infections
- diabetes mellitus
- schizophrenia
- manic depression
- if you are taking diuretics (water tablets)
- if you are undergoing ECT (electroshock treatment)
- if you are going to have surgery or major dentistry: tell your doctor or dentist because Nardil may interact with certain anaesthetics and should not be taken for two weeks before surgery.
Your blood pressure should be monitored frequently by your doctor and Nardil should be stopped if palpitations or frequent headaches occur.
Taking other medicines
Please tell your doctor, dentist or pharmacist if you are taking or have recently taken any other medicines, including medicines obtained without a prescription.
In particular, tell your doctor if you are taking any of the following medicines, because Nardil may interact with them:
- cough and cold cures, cough medicines
- hay fever medications, asthma inhalant medications
- appetite-suppressing medicines, weight-reducing preparations and ‘pep’ pills
- strong pain killers (pethidine and morphine). This could be a serious reaction
- tryptophan, amphetamines and medicines of the type known as sympathomimetic amines (adrenaline, epinephrine, fenfluramine, ephedrine, phenylpropanolamine, dopamine and levodopa). Some of these may be in medicines bought without a prescription
- medicines used to treat high blood pressure (particularly guanethidine)
- diabetes medications
- antimuscarinic medicines, used to treat motion sickness, muscle cramps in the gut or bladder, or Parkinson’s disease
- medicines which make you sleepy (including barbiturates and alcohol) and local anaesthetics including cocaine. The effect of these medicines may be increased by Nardil
- amfebutamone (to help you give up smoking). This should not be taken at the same time as, or within 14 days of, Nardil
- migraine medications known as 5-HT1 agonists. These should not be taken at the same time as, or within 14 days of, Nardil
- medicines to treat epilepsy, altretamine (for ovarian cancer), doxapram (to stimulate breathing in emergency situations), tetrabenazine (for Huntington’s chorea), oxypertine and clozapine (for schizophrenia and other similar illnesses)
- other antidepressants:
- other MAOIs, buspirone or dibenzazepine derivative drugs (e.g. tricyclic antidepressants, perphenazine or carbamazepine), selective serotonin re-uptake inhibitors (SSRIs) or serotonin noradrenaline re-uptake inhibitors (SNRIs, e.g. venlafaxine). Nardil should not be taken for 14 days either before or after these medicines.
- clomipramine or imipramine – 21 days should elapse before starting Nardil.
If you are not sure which medicines you are already taking, please ask your doctor or pharmacist.
Taking Nardil Tablets with food and drink
Nardil tablets react with a substance called tyramine which is found in some foods and drinks (see lists below).
If you eat or drink anything containing tyramine while you are taking Nardil, or within 14 days of taking Nardil, you may have a very severe rise in blood pressure.
This will happen soon after eating the food and you may get a violent headache, pounding heart, stiff neck, flushing, sweating or you may be sick. The severity of the reaction depends on the amount of tyramine you eat and may be mild or could be dangerous, even fatal.
If you feel such a reaction happening, tell your doctor or go to your nearest hospital accident and emergency department immediately.
Do not eat:
Cheese (cooked or plain), liver, yoghurt, yeast/meat extracts (e.g. Marmite, Oxo, Bovril or Brewer’s yeast), flavoured textured vegetable protein, broad bean pods, protein which has been allowed to age, degrade or ferment (e.g. hung game, pickled herrings or dry sausage such as salami or pepperoni), fermented soya bean extract, excessive amounts of chocolate.
Do not drink:
Alcohol, non-alcoholic beer, lager or wine. You may drink a reasonable amount of tea or coffee but not to excess.
Pregnancy and breast-feeding
Nardil is not recommended for use during pregnancy, especially during the first and last trimesters. If you are pregnant, think you might be pregnant or are planning to become pregnant, you should talk to your doctor.
Do not breast-feed if you are taking Nardil.
As with any medicine, ask your doctor or pharmacist for advice.
Driving and using machines
Nardil might cause drowsiness or blurred vision. Do not drive or operate machinery until you know if the tablets affect you in this way.
Important information about some of the ingredients of Nardil Tablets
Sunset yellow (E110), a colouring agent in the film coating of Nardil, may cause an allergic reaction.
Side Effects
Nardil Tablets Side Effects
Side effects are usually mild or moderate in severity and tend to disappear as treatment continues.
The most serious side effects are high blood pressure, which usually happens when the wrong food is eaten (see Section 2 “Taking Nardil Tablets with food and drink”), and neuroleptic malignant syndrome (a serious, sometime life-threatening, condition which results in fever, faster breathing and pulse rate, sweating, muscle stiffness, changes in blood pressure and reduced consciousness). If you feel this is happening to you, STOP TAKING the tablets and tell your doctor or go to your nearest hospital accident and emergency department immediately.
Common side effects are:
- drowsiness, dizziness, weakness, tiredness and blurred vision (see Section 2 “Driving and using machines”)
- low blood pressure when standing or sitting up. You may feel giddy and about to faint. This effect is more common in the elderly
- water retention (can cause swollen ankles)
- nausea, vomiting, dry mouth, constipation
- insomnia (difficulty in sleeping)
- twitching, increased reflexes
- difficulty in achieving an orgasm
- changes in the blood related to liver problems (this may be identified in a blood test)
Uncommon side effects are:
- headache, nervousness, excitement, jitteriness, shaking, confusion, seeing or hearing things which are not there, fits
- changes in normal behaviour, speech changes (repeating the last word of a sentence), unusual eye movements
- loss of feeling in hands and feet
- rash, itching, sweating, nerve pain, bruising
- a feeling of pins and needles
- changes in the rhythm of the heart
- increased appetite and weight
- difficulty in passing urine
- impotence, delayed ejaculation
- high levels of sodium (salt) in the blood, symptoms may be tiredness, weakness, irritability and swelling
- abnormalities of blood cells, symptoms can include bleeding problems, weakness or pale skin colour, or frequent infections
- high pressure in the eye (glaucoma)
- lupus-like illness (a disease affecting the immune system)
- high levels of liver enzymes (this may be identified in a blood test).
Very rarely, other serious effects have been seen, these are:
- loss of co-ordination
- coma (being unconscious) delirium (disorientation, seeing or hearing things which are not there, delusions, and incoherent speech)
- neuroleptic malignant syndrome (a serious, sometimes life-threatening, condition which results in fever, faster breathing and pulse rate, sweating, muscle stiffness, changes in blood pressure and reduced consciousness)
- mania (excessive feeling of well being), rapidly developing anxiety
- schizophrenia, in people already at risk of developing it
- heart and lung problems following electroshock therapy (ECT)
- jaundice (yellowing of the skin), liver damage which may be serious or even fatal
- increased metabolism
- swollen glottis (top of the wind-pipe).
Too little sodium (salt) in the blood has been seen with all types of antidepressants. This may cause drowsiness, confusion or fits. It is more usually seen in the elderly.
If any of these side effects gets serious, or if you notice any side effects not listed in this leaflet, please tell your doctor.
Thoughts of suicide and worsening of your depression or anxiety disorder
If you are depressed and/or have anxiety disorders you can sometimes have thoughts of harming or killing yourself. These may be increased when first starting antidepressants, since these medicines all take time to work, usually about two weeks but sometimes longer.
You may be more likely to think like this:
- If you have previously had thoughts about killing or harming yourself.
- If you are a young adult. Information from clinical trials has shown an increased risk of suicidal behaviour in adults aged less than 25 years with psychiatric conditions who were treated with an antidepressant.
If you have thoughts of harming or killing yourself at any time, contact your doctor or go to a hospital straight away.
You may find it helpful to tell a relative or close friend that you are depressed or have an anxiety disorder, and ask them to read this leaflet. You might ask them to tell you if they think your depression or anxiety is getting worse, or if they are worried about changes in your behaviour.
Reporting of side effects
If you get any side effects, talk to your doctor, pharmacist or nurse. This includes any possible side effects not listed in this leaflet. You can also report side effects directly via the Yellow Card Scheme. Website: www.mhra.gov.uk/yellowcard. By reporting side effects you can help provide more information on the safety of this medicine.
Only logged in customers who have purchased this product may leave a review.
Questions and answers of the customers
- A Nardil 15mg tablets is out of stock until November 2019
Other Products From This Seller
Steglatro Tablets – Ertugliflozin Tablets available in 2 strengths:
- Steglatro 5mg Tablets – Ertugliflozin 5mg Tablets
- Steglatro 15mg Tablets – Ertugliflozin 15mg Tablets
£49.50
- Availability: in stock
Original price was: £43.20.£39.50Current price is: £39.50.
Ursodeoxycholic Acid Tablets 250mg – Cholurso Tablets, 60 Tablets Introducing Cholurso Tablets the brand name of Ursodeoxycholic Acid Tablets 250mg – Your Solution for Gallstone Management and Liver Health Ursodeoxycholic Acid 250mg Tablets is a cutting-edge pharmaceutical formulation designed to positively influence bile composition, making it a versatile solution for various health concerns. Ursodeoxycholic Acid, […]
Learn MoreOriginal price was: £43.20.£39.50Current price is: £39.50.
- Availability: in stock
£156.00 – £210.00
Please note you need insulin pen needles to use Mounjaro Injection
Mounjaro Injection – Tirzepatide Injection, 4 Pre-filled Pens
Available in 6 strengths:
- Mounjaro 2.5mg Injection
- Mounjaro 5mg Injection
- Mounjaro 7.5mg Injection
- Mounjaro 10mg Injection
- Mounjaro 12.5mg Injection
- Mounjaro 15mg Injection
Learn More
£156.00 – £210.00
- Availability: in stock
Timoptol LA Gel – Timolol Eye Gel is available in 2 strengths
- Timoptol LA 0.5% Gel
- Timoptol LA 0.25% Gel
£7.50
- Availability: in stock
Original price was: £43.50.£39.75Current price is: £39.75.
One-Alpha Drops 2mcg/1ml – Alfacalcidol Drops 2mcg/1ml
Learn MoreOriginal price was: £43.50.£39.75Current price is: £39.75.
- Availability: in stock
Original price was: £5.99.£5.39Current price is: £5.39.
Ideal for irrigating and cleansing the eye, or a wound
Learn MoreOriginal price was: £5.99.£5.39Current price is: £5.39.
- Availability: in stock
Ultimate Surefit Erection Ring Set 15222 – Constrictor Rings For Erectile Dysfunction Experience Confidence and Pleasure with the Ultimate Surefit maintenance ring set – Your Key to Intimate Well-being Introducing the Ultimate Surefit Erection Ring, a premium solution meticulously designed for those seeking to overcome the challenges of erectile dysfunction. Crafted with precision and comfort […]
Learn More£58.50
- Availability: in stock
Original price was: £62.50.£56.49Current price is: £56.49.
SureEase Erection Rings 15085 – Constrictor Rings For Erectile Dysfunction Revitalize Your Intimate Moments with SureEase Erection Rings – Precision for Confidence and Pleasure SureEase Erection Rings are the discreet yet powerful solution designed to rekindle confidence and elevate pleasure for individuals facing challenges with erectile dysfunction. Crafted with precision, these constrictor rings provide targeted […]
Learn MoreOriginal price was: £62.50.£56.49Current price is: £56.49.
- Availability: in stock
£279.00 – £289.00
SomaErect Response II is available in 2 models:
- SomaErect Response II 15019
- SomaErect Response II XL 15888
£279.00 – £289.00
- Availability: in stock
Original price was: £331.50.£289.90Current price is: £289.90.
SomaErect Touch II 15013 – Vacuum Pump Erection Device Introducing SomaErect Touch II 15013 – Redefining Intimacy with Advanced Vacuum Pump Technology The SomaErect Touch II 15013 is an innovative vacuum pump erection device, meticulously engineered to provide a discreet, effective, and user-friendly solution for individuals dealing with erectile dysfunction. Embrace confidence and intimacy with […]
Learn MoreOriginal price was: £331.50.£289.90Current price is: £289.90.
- Availability: in stock
















8 reviews for Nardil 15mg Tablets – Phenelzine, 100 Tablets
There are no reviews yet.